April 2019, Basel, Switzerland: A large study just published in the journal Anaesthesia raises important questions about the way anaemia is currently managed in surgical patients (Associations of nadir haemoglobin level and red blood cell transfusion with mortality and length of stay in surgical specialties: a retrospective cohort study). Professor Jeffery Hamdorf, Winthrop Professor of Surgical Education at The University of Western Australia and Chairman of the Western Australia Patient Blood Management Group, commented “This study will change the way people think about transfusion and haemoglobin levels.”
Anaemia (lower than normal levels of haemoglobin in the blood) is associated with adverse patient outcomes. Transfusion has been the traditional treatment for moderate to severe anaemia, with the patient’s haemoglobin level being the primary consideration in the decision to transfuse. Questions, though, have been raised within the medical community in recent years about the effectiveness of transfusion (Appropriateness of Allogeneic Red Blood Cell Transfusion: The International Consensus Conference on Transfusion Outcomes).
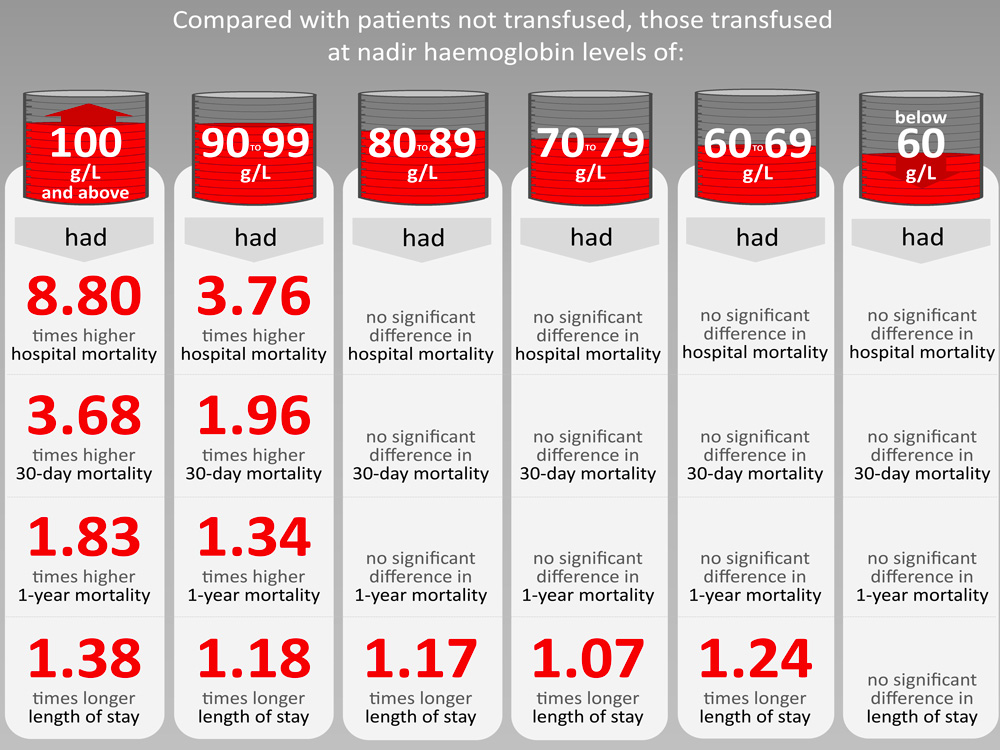
Researchers from The University of Western Australia looked at over 60,000 patients undergoing surgery to determine if there is a level of anaemia where transfusion is effective. After adjusting for patient risk factors, they found that transfusion did not reduce the risk of death at any level of anaemia and was associated with longer hospital stays.
Study co-author Shannon Farmer, Adjunct Research Fellow at the University of Western Australia, said “Research shows if you are admitted to hospital anaemic your risk of adverse outcomes, including the risk of death, is increased and increases incrementally if your anaemia becomes more severe. While confirming that, this study found that receiving a transfusion did not reduce the risk of death compared with those who did not receive a transfusion, regardless of the severity of anaemia.”
Improved management of patients’ anaemia has become an important focus in the global uptake of patient blood management (PBM) programs. A landmark study evaluating the results of the world’s first health-system-wide PBM program reported fewer deaths and complications, and shorter hospital stays with this approach (Improved outcomes and reduced costs associated with a health‐system–wide patient blood management program: a retrospective observational study in four major adult tertiary‐care hospitals). The current study highlights the urgent need for a greater focus on preventing the development of anaemia and, when it does develop, exploring more appropriate methods of managing it. A recent editorial in the journal Annals of Surgery stated, “not implementing patient blood management represents substandard care.” (Patient Blood Management What Else?)

